In the evaluation of male fertility through the analysis of a semen sample under a microscope, the desired outcome is to see a lot of “good swimmers” among the spermatozoa – although this still says little or nothing about their morphology and inner structure. Thanks to modern technologies, it is now possible to go into this in greater detail. This is done by extending semen analysis beyond the existing WHO criteria by adding so-called molecular diagnostics.
WHO criteria to serve as the basis
A spermiogram (semen analysis) implies an analysis of the ejaculate on the basis of standardized investigation methods and associated reference values laid down by the World Health Organization (WHO).
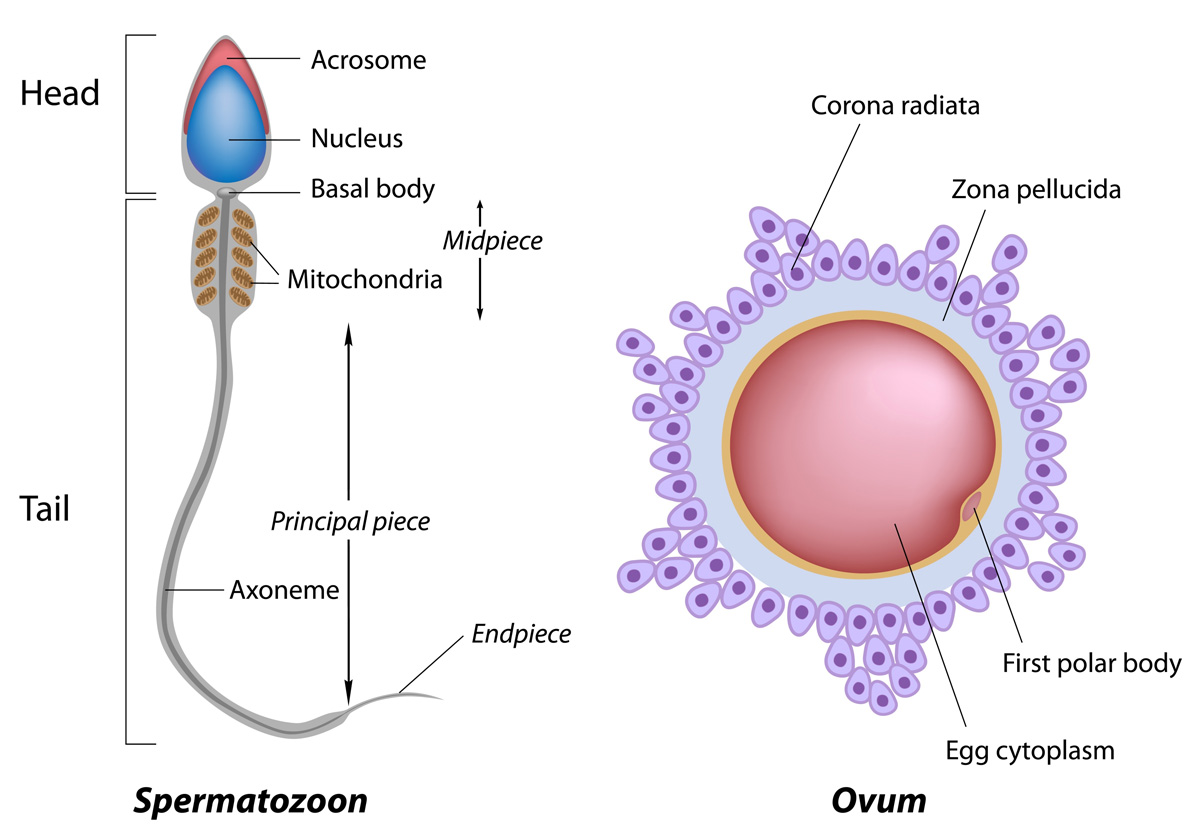
This spermiogram forms the foundation and provides a first overview of the situation as regards concentration, motility, vitality, structure and morphology of the spermatozoa. However, when dealing with involuntary childlessness, these parameters alone may not be sufficient for reliable detection of male factor infertility. Read more…