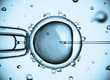
“After my wife’s oocytes had been fertilized by my sperm and some of the impregnated ova have developed into embryos, we now want to know which embryo is the one most suitable for being transferred to the uterus and what our chances are to achieve a pregnancy and the birth of a healthy child.“
What matters most to these intended parents – and what they share in common with many others – is that they want to know more about the development of their embryos. Embryo formation is probably one of the most important steps in the course of an IVF treatment. In order to evaluate the developmental potential of embryos prior to performing embryo transfer, the professional knowledge of experienced biologists is needed. Such assessment can be supported by using an assistive tool – the so-called “Time-Lapse Analysis”, which allows for monitoring embryonic development by means of time-lapse imaging using a special camera system (e.g. EmbryoScope). Subsequently, the embryo with the highest implantation potential (Single-Embryo-Transfer) is to be determined on the basis of pre-established criteria. This approach, of course, raises some questions:
Could it happen that embryos whose early development has to be regarded as suboptimal are nevertheless able to result in pregnancy and the birth of a healthy baby?
Moreover, can it be justified that instead of transferring these embryos, the focus is put on the success of a subsequent future IVF cycle – an attempt with an uncertain outcome?
To answer these questions, a study was carried out. The results have been published in the renowned scientific journal RBM Online. The study shows how important it is to do research in this field of reproductive medicine.
The analysis includes various case studies, in which at least one of the transferred embryos at or up to the blastocyst stage (development until the 5th day following in vitro fertilization) has not met the criteria to be classified as the most suitable for transfer.
Achieved result: All transfers have led to intact pregnancies and the birth of healthy children!
Conversely, this means that standard exclusion criteria need to be treated with caution. Even though some of these embryos are associated with a reduced implantation potential, this does not mean that the chances of getting pregnant and giving birth to a healthy child are equal to zero! An embryo that does not meet certain criteria on the 2nd and 3rd day of its development or whose development is retarded can nevertheless reach the blastocyst stage and develop into a healthy child after being transferred to the uterine cavity!
“Time-Lapse” – development, assessment, implantation?
In order to help childless couples to fulfill their heart’s desire, the goal of any treatment at the
IVF Centers Prof. Zech is to transfer the best-developed embryo (= high implantation potential and no genetic impairment), while adhering to the highest quality standards in terms of technology and science.
Therefore, the selection of the so-called gametes (oocytes and spermatozoa) and subsequently that of the embryos is performed on the basis of mostly morphological criteria, i.e. by assessing form and structure. It is important to note that due to different legal provisions, the possibilities in the field of reproductive medicine may vary from one country to another (this may also involve embryo selection/blastocyst selection).
When selecting the most suitable embryo for transfer, so-called IVF incubators with integrated camera systems are, among others, used for the assessment. Those camera systems allow for continuous and undisturbed image documentation during embryonic development in in-vitro culture (e.g. EmbryoScope, “Primovision” or similar devices). Such incubators with monitoring function permit a detailed recording of any changes by means of time-lapse shots. This dynamic monitoring system is by far superior to static monitoring.
Since the first steps were taken towards developing this method – whereby the IVF Centers Prof. Zech have played a vital part (first studies by top biologists such as Dr. Pierre Vanderzwalmen who has been with the “Zech-Group” since 1994) – numerous scientific papers on the issue have been published worldwide and various indicators have been established. These indicators are used to evaluate the embryo’s chances to successfully implant into the uterine cavity.
However, as the aforementioned study demonstrates, these indicators need to be subjected to close scrutiny. Moreover, as regards embryonic development, the focus of future research projects will be on the so-called paternal effect, i.e. the impact of male sperm (more details in one of our next blog posts).
The results are intended to provide orientation
To sum up, it can be noted that, given the current state of scientific knowledge in the field of reproductive medicine, embryos that are cultured to the blastocyst stage (day 5) allow for the best-possible assessment of their development potential.
Furthermore, the demonstrated research results should raise awareness of the fact that rejecting embryos on the basis of analysis results obtained during an early stage of development cannot be deemed to be a purposeful approach also in view of the possibilities opened up by cutting-edge freezing techniques. On the contrary, we believe it may even add to the physical and psychological stress as well as to the financial burdens of the couples concerned. It is therefore all the more important to have a sound clarification of relevant medical findings of both partners in a couple and to offer treatment that is tailored to their individual situation in order to achieve a pregnancy and the birth of a healthy child – “if possible as early as the first IVF cycle”.
→ more articles concerning this topic in the Special »Why embryo implantation did not take place – Possible causes and treatment-options«
← Home
→ Contact